Sian Jones and Monika Rusieka
Red Kite Health Solutions CIC, Powys
Project Background:
Chronic pain affects one-third to one-half of the population in the UK, accounting for 22% of all primary care visits. The demand for appointments is at an all-time high, with opioid prescribing in Wales increasing by 30% over the last decade. Patients often visit their GP for help, but due to the limitations of a 10-minute appointment, it becomes difficult to thoroughly assess the patient’s condition, establish a good rapport, or ensure continuity of care. This leads to inefficient use of GP appointments and sub-optimal patient care.
Project Aims:
- To introduce a primary care pain management service focused on improving the quality of life for individuals
- Influence opioid/gabapentinoid prescribing cultures
- Develop a new MDT role to provide education for patients and clinicians
Project Impact:
- 75 min of GP time saved per patient
- 630 extra GP appointments available
- £21,735 of clinical time avoided
- Improved patient care
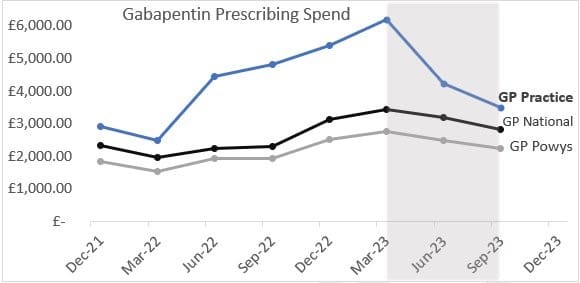
- 44% reduction in Gabapentin prescribing
Feedback:

Patient Story:
When I turn in bed, I wake in pain, so I get up because I’m fully awake regardless of if I’ve only been sleeping for 45 mins or a couple of hours. I sit up in bed and I get shooting pains. My cheeks flush with anger and I curse and swear at the pain as if it’s a living entity. I hesitate before I move as I know it’s going to hurt like hell. I count in my head 1.2.3 {insert curse word here} as almost every motion has its own personal “hurt”. My neck, both shoulders, both knees & lower back all in varying degrees of pain and all have various swear words associated, from the mildest for my left shoulder, to the vilest for my back. I get up, make a cup of tea, and stay up, generally all night until I feel absolutely exhausted and go back to bed.
It’s exhausting, depressing, hopeless, frustrating, makes me feel completely inadequate because I can’t do the simplest of tasks. The worse it gets, the less I do & the less I do, the worse it gets. I psych myself up for days sometimes, just to go to the shop for essentials, often running out of milk, bread etc. but I manage without until I can go. Mental health plays a big part in this too, so it’s not just the pain preventing me from doing things. I dread going out because I know before I get home, I’ll be in awful pain. Some of the pain is sharp enough to sicken me, some is minor, some medium, but all combined is almost too much to put up with. I have massive walls to climb before I manage a moderate exercise regime and start losing weight, which I’m almost certain will help with at least some of the pain. I am trying to control the pain rather than letting it control me, but I’m losing the fight at the moment.
Does M and the service make a difference? When we 1st spoke, I was very guarded and wary of M, thinking this was just another do gooder, nosey busybody trying to save the NHS money and leave me in pain with no meds. Well, I soon realised that I couldn’t have been more wrong. It takes a long time for me to trust someone, especially someone I have never met. But I knew very quickly that the practitioner had my very best interests at heart, and she was going to help. Not only does she make sure I am on the right medication and proper dosage for my physical issues, but she also takes the time to talk in general and to ensure I’m in the best place mentally.
I cannot stress how important the service and help that M gives to me is. We are working together to try and reduce my medication currently, and also improving my mental health. Through M’s persuasion I started speaking to MIND and I’m trying to change & improve my way of life. I hardly leave my home at the moment because of pain and mental health, but I am making small changes to improve things. This is all thanks to the service.
Project Outcomes:
- A new service was introduced in two South Powys locations for patients with persistent pain, improving their quality of life.
- There has been a significant impact on prescribing culture, leading to an average 42% reduction in Gabapentin and Tramadol prescriptions, associated costs and improved patient safety.
- Our service has saved GP time, and improved the patient experience, increasing the quality of care.





