Shirley Jonathan and Leah Watson
Swansea Bay University Health Board
Background:
On a yearly basis, there are 200+ preschool children (under 5) across the health board who need an assessment to determine whether they are on the Autistic Spectrum.
Due to the impact of social communication needs and neurodevelopmental conditions, including Autism, early diagnosis for these children is crucial as it often gives access to specialist services and support for the families. It is well documented that children and people with Autism face inequalities. More recently, the Left Stranded report (2020, National Autistic Society) has highlighted this.
A diagnosis is important to determine a child’s ongoing Additional Learning Needs (ALN) to guide school staff to their provision under the ALN Reform (commencing September 2021).
Receiving a diagnosis of Autism can open many doors for a family and child to receive much needed support and early intervention.
In 2020, there was a disruption in services and the gold standard assessment that we usually utilize, the Autism Diagnostic Observation Schedule (ADOS), is not standardised with the social partner wearing a mask and so could not be used.
We were keen to keep the flow of children moving through the Early Years Neurodevelopment assessment pathway. So, we adapted and developed new ways of carrying out the autism diagnostic assessments with preschool children and their families.
This included:
- Telehealth Parent interview / discussion carried out by the Paediatrician.
- A Specialist Speech and Language, Social Communication Telehealth Assessment, based on the individual needs of each child.

Table 1: Examples of the techniques used for children who are not using any or many words.

We utilized a novel, shorter assessment tool specially devised for use during the Covid-19 pandemic. This required parent coaching, thereby empowering them to be the social partner, rather than the professional and allowing them to carry out the interaction mask free.
This is called the Brief Observation of the Symptoms of Autism – (BOSA) developed by the UCLA based on the Autism Diagnostic Observation Schedule. For more information and the training video click here.
These sessions were carried out by a Paediatrician and Specialist Speech and Language Therapist.
We are collaborating with the UCLA on this project and contributing to the validation of this tool.
These methods comprise our toolkit and allow us to select the right approach for each family’s circumstances and child’s needs.
- A new pathway was formed that includes a multi-professional consensus case discussion for each child, to decide the diagnostic outcome.
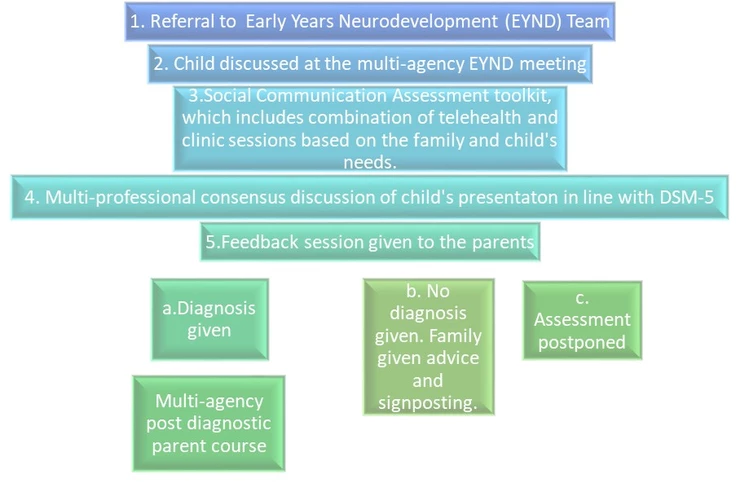
The team of people who carry out the early years neurodevelopment assessments consists of Paediatricians and Speech and Language Therapists.
Project Aims:
To continue the flow of Autism assessments in the Early Years population during the Covid-19 pandemic, by implementing a prudent pathway, moving telehealth to the forefront and increasing parent participation and co-production.
To provide timely, valid and quality Autism assessments in line with best practice and national guidelines, within the context of the global pandemic.
To make long-term improvements to the service by:
- Reviewing the assessment pathway, following the pilot and making revisions based on our findings and to support the reduction of wait times from referral to diagnosis.
- To enhance the families’ overall experience of the assessment pathway by analysing parental feedback from digital questionnaires.
- To identify risk factors and markers that would help us predict which children require a face-to-face appointment based on language skills, neurodevelopmental features and gender, in line with the existing evidence base in relation to telehealth autism assessments.
- This will help us personalise the child and family’s assessment journey.
Challenges:
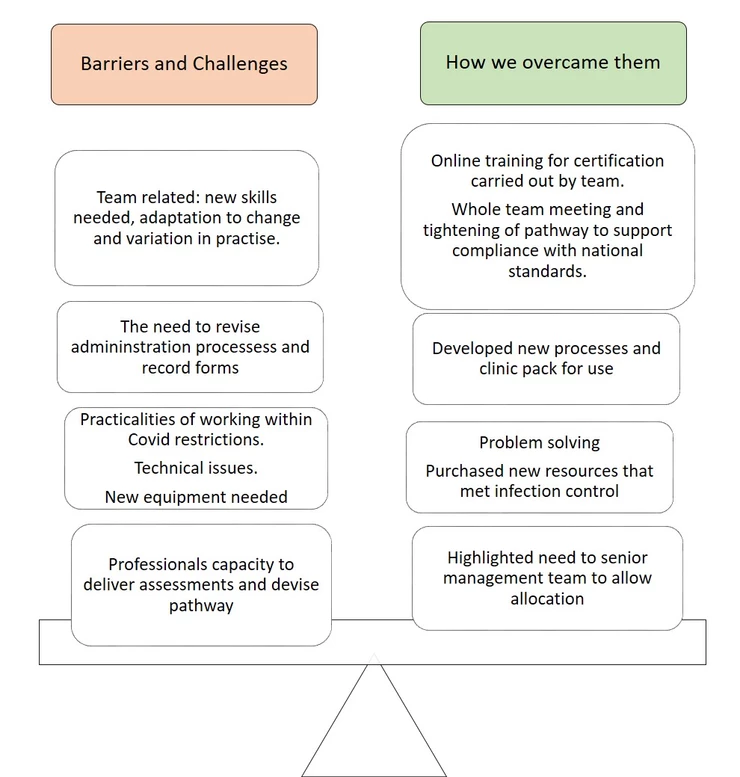
Key Outcomes:
From September 2020 to March 2021:
We were able to reach a diagnostic outcome for 85 children. Of those 74 received a diagnosis of autism. Without our new approaches, these children would have remained on the waiting list.
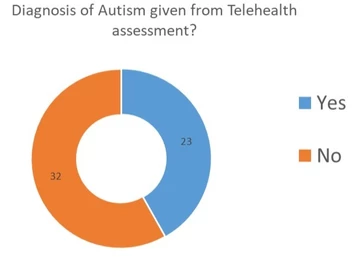
The new clinic assessment allowed us to conclude outcomes for 62 children.
- 51 children were given diagnosis of Autism
- 9 children were given the feedback that their primary needs were language disorder or global developmental delay
- 2 assessments were incomplete
Parent Experience:
Social Communication telehealth feedback
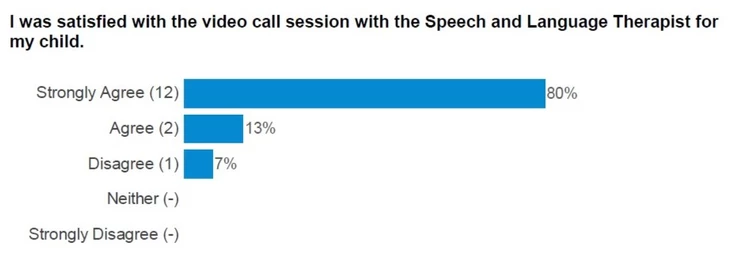
85% of parents who completed the questionnaire ‘strongly agreed’ or ‘agreed’ that their child’s communication and interaction needs, difficulties and strengths were understood by the Speech and Language Therapist.
All of them, with the exception of one, said that they would recommend the session to those with similar needs.
“You can get a good idea of her behaviour when she is her own environment and acts more naturally.”
Parent
Face-to-face clinic assessment feedback:
95% of parents who completed the questionnaire agreed with their child’s diagnostic outcome.

Next Steps:
Going forward we want to explore the clinical markers to decide which children are likely to need face-to-face assessment and which ones can be offered telehealth in the first instance. For example, we have found that in this pilot project, that those children with sentence language level with a mixed presentation have needed a face-to-face assessment.
When we asked parents who had received both clinic and telehealth appointments where they would like their child seen in the future. Their choices were as follows:
- 14 said Mixture of both
- 20 said Clinic appointment (based on new assessment)
- 2 said Video call appointment from home
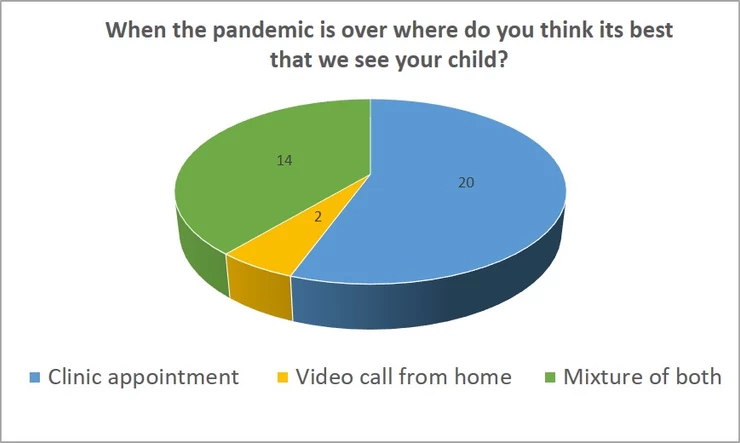
It would be beneficial to revisit this feedback with a larger group. Going forward, we would envisage carrying out a mixture of both telehealth and clinic to support patient choice, balanced with our capacity to reduce the waiting times overall.
There are possible opportunities to undertake a research project in collaboration with Swansea University.
We also have plans to strengthen our support and intervention for children and their families pre and post diagnosis. This includes a new speech and language therapy programme for parents and child, as soon as social communication needs are identified.
Showcase:
Contact:
Dr Shirley Jonathan: 01792 517950
Mrs Leah Watson: 01792 517865



