Steve Hill
Velindre NHS Trust
Context:
Imagine: You have been diagnosed with cancer, and then you have been told it is not curable and treatment is now palliative. Imagine one day that you are suffering with a multitude of symptoms, and the medication does not help.
You need radiotherapy (RT), and your treatment is scheduled sometime within the next two weeks. How would this affect your quality of life? Could you do the things you want to do? With time being short.
Any solution needed to have a patient centred approach, involving everyone as equally as possible without demanding too much of the patients precious time.
In Velindre Cancer Centre (VCC), approximately 1621 patients per year are receiving palliative radiotherapy, (1341 palliatives and 280 emergency patients), which is approximately 39.7% of total radiotherapy patients in VCC and 7355 fractions (sessions) of RT. A recent telephone palliative patient experience survey carried out at VCC asked what symptoms they experienced and found 45% of patients have had symptoms for over 3 months, while 69% having had their symptoms over one month.
Planning and Development:
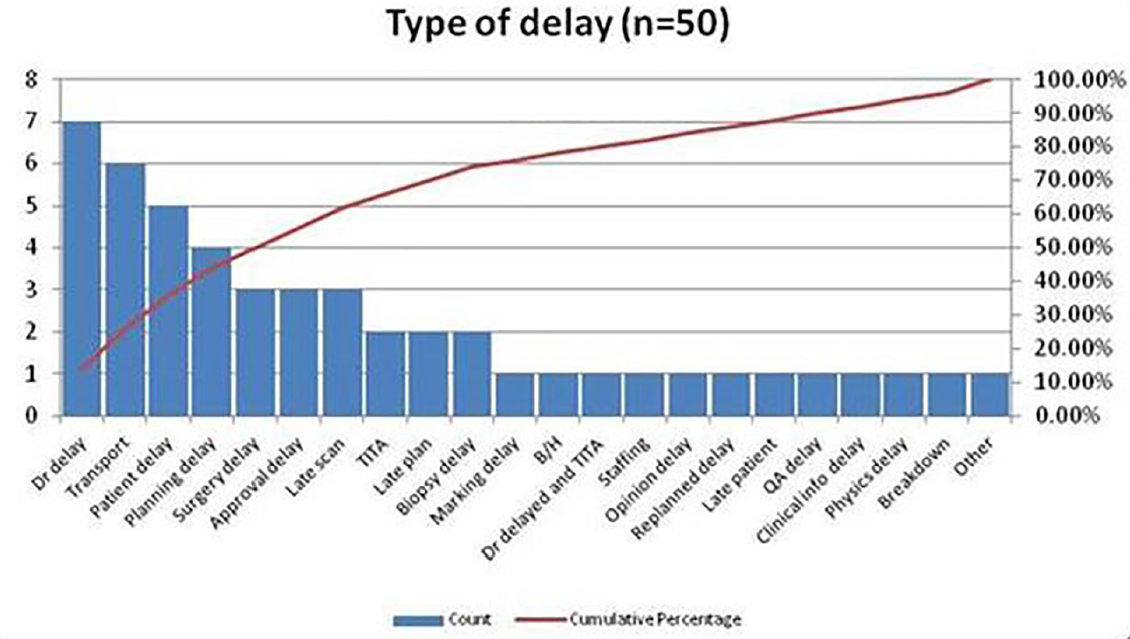
Identifying what problems the patients were facing and why they were delayed helped the team identify where the greatest need was first four months worth of data was then collected and analysed along with swimlane mapping and calculating Opportunity Costs for past, present and future developments.
Key findings:
The Royal College of Radiologists (RCR) recommend the gold standard from referral to starting RT for all emergencies is 24 hours (acceptable is 48 hours) and palliatives is 2 days (accepted is 14 days) (RCR, 2005).
The service at VCC before May 2016 delivered an average referral to starting RT time for emergencies of 1.14 days and 5.45 days for palliative patients. Although acceptable, it was found this causes a disruption 51 % of the time to a busy Outpatient department. The palliative radiographer and team at VCC identified a need to develop a rapid-access service onto Palliative Radiotherapy, to reduce the wait from referral to treatment time (RTT) with little or no disruption to outpatients and deliver the expected quality of care. This was piloted from May 2017.
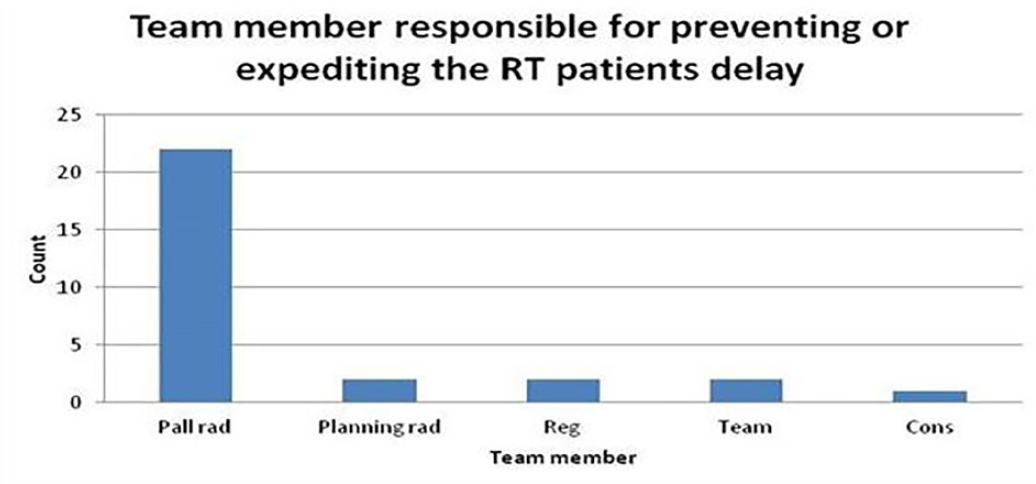
Data analysis showed that days the palliative radiographer undertook tasks on behalf of the medic had significantly shorter cycle times and expedited delays.
Future:
By adopting more of the roles traditionally performed by the medical staff could further reduce RTT. This scenario has been swimlane mapped and an opportunity cost analysed.
Further development of an advanced palliative radiographer role across Wales to further improve patient experience and reduce disruption to outpatients could save £211,224 per year at least.



