David Minton, Anne Sprackling, John Dicomidis
Aneurin Bevan University Health Board
Aim:
To reduce medicines waste in care homes through improving the efficiency of medicines ordering.
Context:
- Perceived waste of medicines through: over ordering by care home staff; over prescribing by GPs; overly complicated ordering process via community pharmacy; and,
- Historical work on practice prescribing not altered probable over-prescribing.
Planning:
- Introduce alternative way of homes ordering ‘as required’ medications; make routine medication ordering more efficient to give confidence to care home staff that when medication is ordered it will be delivered expediently; and,
- Use MHOL to improve ordering process, speeds ordering up, removes initial step of MAR chart going to pharmacy before prescription request arriving at GP practice. Reduces risk of practice issuing script not required.
Measurement:
- Measure level of waste.
- Homes record waste – nursing homes with reason for waste.
- Measure change in wastage.
- Measure ‘urgent’ script requests if possible.
- Time to order prescription.
- Time to process prescriptions.
Impact and benefits:
- Reduce waste = reduce cost.
- Reduce over ordering = reduction in workload for both practices and pharmacies.
Waste cost per resident (left), and average monthly waste (right) before & after:
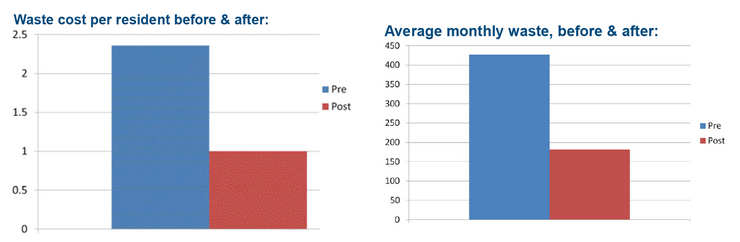
- Increase ownership and understanding of medicines amongst staff = reduction in potential harm to residents.
- Less time at every step in process.
- Feedback from homes to influence future uptake.
- Measure after 6 months to prove waste reduction. If confirms then approach other homes within BGW NCN and other NCNs, further afield as feasible.
Next Steps:
- Proof of concept.
- Roll out to more homes.
- Measure time to prove anecdotal time saving.
- Influence MHOL development – e.g. home can log on once rather than for each patient.
- GP practice views first line of patient address and can view by address.
- Further measurement of waste.
Fit with Prudent Health:
- By improving the efficiency of repeat prescribing ordering in care homes there is a lesser chance of residents receiving medications unnecessarily and thus reducing harm.
- Potential reduction in costs.
- Greater ownership of the patient’s medication by the carers in the home and through education of staff a greater understanding of the residents’ medications and further reduction of harm risk.
- Reduced inefficiencies in pharmacies and practices allowing staff to focus on patient care by not being diverted to ‘unnecessary’ work.
- There is only one step in the ordering process, making identification of any issues possible at an earlier stage.



